Navigating the labyrinth of healthcare expenses often begins with a fundamental question: how much does health insurance cost? This seemingly simple query unlocks a complex web of variables, from age and location to the type of plan chosen and the availability of government assistance. Understanding these factors is crucial for making informed decisions and securing the most cost-effective coverage. This guide aims to demystify the complexities, providing a clear roadmap to understanding and managing your health insurance costs.
The cost of health insurance is influenced by a multitude of elements. Age plays a significant role, with premiums generally increasing as individuals get older. Location also impacts costs due to variations in the local healthcare market and the cost of medical services. The type of plan, such as HMOs, PPOs, or HDHPs, dictates the network restrictions, cost-sharing arrangements, and overall premium levels. Lifestyle choices, including smoking and pre-existing conditions, further contribute to premium fluctuations. Furthermore, government subsidies and financial assistance programs can significantly reduce the financial burden, making health insurance more accessible for many individuals and families.
Understanding the Fundamental Factors That Influence Health Insurance Premiums.
Health insurance premiums, the regular payments for coverage, are not arbitrary. They are calculated based on a complex interplay of factors that reflect an individual’s risk profile and the anticipated cost of their healthcare needs. Understanding these factors is crucial for consumers to make informed decisions and choose a plan that aligns with their financial situation and healthcare requirements. This involves assessing the impact of age, location, the type of plan, lifestyle choices, and pre-existing conditions.
Age, Location, and Plan Type: Key Drivers of Health Insurance Costs
Several key variables significantly influence the cost of health insurance premiums. These include the age of the insured, the geographic location where they reside, and the specific type of health insurance plan selected. Each of these factors contributes differently to the overall premium cost, reflecting varying levels of risk and anticipated healthcare utilization.
Age is a primary determinant of health insurance costs. Generally, premiums increase with age, reflecting the increased likelihood of health issues and higher healthcare consumption as individuals get older. For instance, a 30-year-old in a major metropolitan area might pay around $400 per month for a mid-level plan, whereas a 50-year-old with similar coverage could face premiums of $700 or more. This disparity is because older individuals are statistically more prone to chronic conditions, require more frequent medical visits, and are more likely to need prescription medications. Conversely, younger, healthier individuals often pay lower premiums, reflecting their lower risk profile.
Geographic location also plays a significant role in determining health insurance premiums. Healthcare costs vary widely across different regions due to factors such as the cost of living, the availability of healthcare providers, and the competitive landscape of the insurance market. For example, premiums in states with higher healthcare costs, such as New York or California, might be significantly higher than those in states with lower costs, such as South Dakota or Mississippi. This is because the cost of medical services, hospital stays, and specialist consultations varies substantially from one location to another. Insurance companies adjust premiums to reflect these regional differences, ensuring they can cover the anticipated healthcare expenses of their policyholders in a specific area.
The type of health insurance plan chosen also directly impacts the premium cost. Plans are categorized based on their cost-sharing structure, which determines how much the insured individual pays out-of-pocket for healthcare services. Bronze plans, for example, typically have the lowest monthly premiums but the highest deductibles and out-of-pocket maximums. This means that while the monthly payments are lower, the insured person will pay a larger share of their healthcare costs before the insurance coverage kicks in. Platinum plans, on the other hand, offer the highest monthly premiums but the lowest deductibles and out-of-pocket maximums, providing the most comprehensive coverage and reducing the insured’s financial burden for medical expenses. The choice of plan is a trade-off between monthly premium costs and the level of cost-sharing, directly influencing the overall expense of health insurance.
Deductibles, Co-pays, and Coinsurance: Understanding Cost-Sharing Mechanisms
Health insurance plans incorporate various cost-sharing mechanisms that affect the consumer’s out-of-pocket expenses. These mechanisms, including deductibles, co-pays, and coinsurance, define how the financial responsibility for healthcare costs is divided between the insurer and the insured. Understanding the implications of each mechanism is crucial for consumers to effectively manage their healthcare expenses.
- Deductible: The deductible is the amount a policyholder must pay out-of-pocket for covered healthcare services before the insurance plan begins to pay. For example, if a plan has a $2,000 deductible, the insured must pay the first $2,000 of their healthcare expenses before the insurance company contributes. Higher deductibles typically result in lower monthly premiums, but they also mean the insured bears a greater financial responsibility for initial healthcare costs. This can be advantageous for individuals who anticipate minimal healthcare needs, but it can be a significant financial burden for those with chronic conditions or frequent medical visits.
- Co-pay: A co-pay is a fixed amount the insured pays for specific healthcare services, such as a doctor’s visit or a prescription medication. For instance, a plan might have a $25 co-pay for each primary care visit. Co-pays are paid at the time of service, and they do not count towards the deductible. Co-pays offer predictable costs for common healthcare services, making it easier for individuals to budget for their healthcare expenses.
- Coinsurance: Coinsurance is the percentage of healthcare costs the insured pays after the deductible has been met. For example, if a plan has an 80/20 coinsurance, the insurance company pays 80% of the cost of covered services, and the insured pays 20%. Coinsurance, like co-pays, is paid after the deductible is met. It can significantly impact out-of-pocket costs, particularly for expensive procedures or hospitalizations.
Lifestyle Choices, Pre-existing Conditions, and Premium Impact
Lifestyle choices and pre-existing health conditions can significantly influence health insurance premiums. Insurance companies assess these factors to evaluate the risk an individual poses and adjust premiums accordingly. This assessment is crucial for maintaining the financial sustainability of the insurance pool.
Lifestyle choices, such as smoking, can lead to higher premiums. Smoking is a well-established risk factor for numerous health problems, including heart disease, cancer, and respiratory illnesses. Insurance companies recognize this increased risk and often charge smokers higher premiums to account for the anticipated higher healthcare costs associated with smoking-related illnesses. The premium increase for smokers can be substantial, sometimes adding hundreds of dollars to the monthly premium. For instance, a smoker might pay up to 50% more than a non-smoker for the same health insurance plan.
Pre-existing conditions, which are health problems that existed before the individual enrolled in the health insurance plan, also impact premiums. While the Affordable Care Act (ACA) has prohibited insurance companies from denying coverage or charging higher premiums based on pre-existing conditions, the cost of treating these conditions is still factored into the overall risk assessment and premium calculations. Insurance companies may use the information on the applicant’s health status to determine the level of coverage and the premium rates. The overall effect is that individuals with pre-existing conditions may face higher premiums, particularly for plans that offer more comprehensive coverage.
Exploring the Different Types of Health Insurance Plans and Their Associated Costs
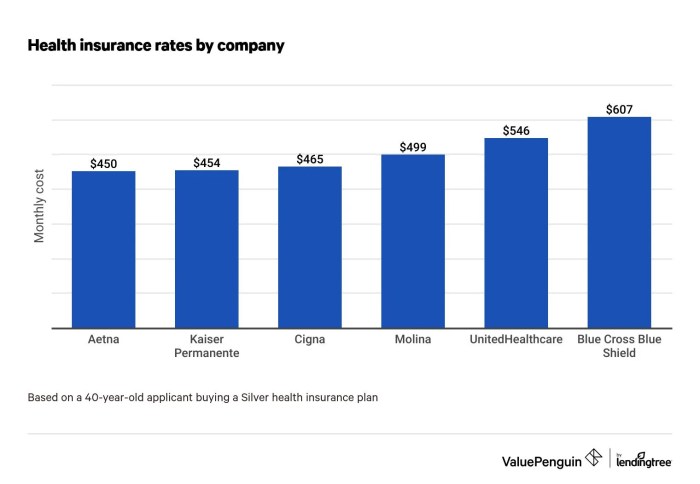
Navigating the world of health insurance can feel like traversing a maze. Understanding the different plan types and their associated costs is crucial for making informed decisions. Choosing the right plan can significantly impact your access to care and your financial well-being. This section delves into the nuances of various health insurance plan options, comparing their features, costs, and network restrictions.
Comparing HMOs, PPOs, EPOs, and POS Plans
The structure of a health insurance plan heavily influences both access to healthcare providers and the associated costs. HMOs, PPOs, EPOs, and POS plans each offer a distinct approach.
- Health Maintenance Organizations (HMOs): HMOs typically offer the most affordable premiums but come with the most restrictive networks. Members must choose a primary care physician (PCP) who coordinates their care and provides referrals to specialists within the network. Out-of-network care is generally not covered, except in emergencies.
- Preferred Provider Organizations (PPOs): PPOs offer greater flexibility than HMOs. Members can see any doctor or specialist without a referral, although costs are lower when using in-network providers. Out-of-network care is covered, but at a higher cost.
- Exclusive Provider Organizations (EPOs): EPOs combine aspects of HMOs and PPOs. They typically offer lower premiums than PPOs, but members must use providers within the network. Unlike HMOs, referrals are usually not required to see a specialist.
- Point of Service (POS) Plans: POS plans combine features of HMOs and PPOs. Members choose a PCP who coordinates care and provides referrals. They can also see out-of-network providers, but at a higher cost and often with a deductible.
The following table summarizes the key differences:
| Plan Type | Network Restrictions | Referral Required? | Out-of-Network Coverage | Typical Premium |
|---|---|---|---|---|
| HMO | Very Restrictive | Yes (for specialists) | Generally not covered | Lowest |
| PPO | Less Restrictive | No | Covered, but at higher cost | Higher than HMO |
| EPO | Restrictive | No | Generally not covered | Mid-range |
| POS | Less Restrictive | Yes (for specialists) | Covered, but at higher cost | Mid-range |
High-Deductible Health Plans (HDHPs) and Health Savings Accounts (HSAs)
High-deductible health plans (HDHPs) are characterized by their lower premiums and higher deductibles. These plans are often paired with health savings accounts (HSAs), which offer significant tax advantages.
- Features of HDHPs: HDHPs typically have lower monthly premiums compared to traditional plans. However, individuals must pay a higher deductible before the insurance company starts covering healthcare costs. After the deductible is met, the plan typically covers a percentage of the costs, and the individual pays the remaining coinsurance until the out-of-pocket maximum is reached.
- Health Savings Accounts (HSAs): HSAs are tax-advantaged savings accounts used in conjunction with HDHPs. Contributions to an HSA are tax-deductible, the money grows tax-free, and withdrawals for qualified medical expenses are also tax-free.
- Tax Benefits: The combination of an HDHP and an HSA provides substantial tax benefits. Tax deductions are available for contributions, the money grows tax-free, and withdrawals for qualified medical expenses are tax-free. This can significantly reduce the overall cost of healthcare.
- Potential Risks: The primary risk associated with HDHPs is the higher out-of-pocket costs before the deductible is met. This can be problematic for individuals with significant healthcare needs or unexpected medical expenses. Planning and budgeting are essential when choosing an HDHP.
Plan Comparison Scenario: Family of Four
Consider a family of four (two adults and two children) evaluating three different health insurance plans: an HMO, a PPO, and an HDHP. The following demonstrates how costs vary:
HMO:
- Monthly Premium: $800
- Deductible: $2,000 per family
- Out-of-Pocket Maximum: $6,000 per family
PPO:
- Monthly Premium: $1,200
- Deductible: $4,000 per family
- Out-of-Pocket Maximum: $8,000 per family
HDHP:
- Monthly Premium: $600
- Deductible: $7,000 per family
- Out-of-Pocket Maximum: $8,500 per family
- Paired with an HSA: Family can contribute up to the IRS limit ($7,750 for 2023)
In this scenario, the HMO offers the lowest monthly premium but the most restrictive network. The PPO has a higher premium but greater flexibility. The HDHP has the lowest premium but the highest deductible. The best choice depends on the family’s healthcare needs and risk tolerance. If the family is generally healthy, the HDHP with an HSA might be the most cost-effective option. If the family anticipates needing frequent medical care, the PPO might be the better choice, despite the higher premium.
Investigating the Impact of Government Subsidies and Financial Assistance on Health Insurance Costs
The cost of health insurance can be a significant financial burden for many individuals and families. Recognizing this, the government offers various forms of financial assistance to help make coverage more affordable. These subsidies and programs are designed to lower the monthly premiums and out-of-pocket expenses for eligible individuals, ensuring access to essential healthcare services. This section delves into the specifics of these financial aid mechanisms, exploring their structure, eligibility requirements, and the impact they have on reducing healthcare costs.
Affordable Care Act (ACA) Subsidies: Reducing Health Insurance Costs
The Affordable Care Act (ACA) introduced a system of subsidies to make health insurance more accessible and affordable. These subsidies, also known as premium tax credits and cost-sharing reductions, are available to individuals and families who meet specific income requirements and purchase health insurance through the Health Insurance Marketplace.
The primary goal of the ACA subsidies is to lower the monthly premium payments for eligible individuals. These subsidies are calculated based on a sliding scale, with individuals and families with lower incomes receiving larger subsidies, thus reducing the cost of their monthly premiums.
The eligibility for ACA subsidies is primarily determined by household income, relative to the Federal Poverty Level (FPL). Individuals and families with incomes between 100% and 400% of the FPL are generally eligible for premium tax credits. The Marketplace calculates the subsidy amount based on the second-lowest-cost Silver plan available in the individual’s area. The subsidy then covers a portion of the premium for any Marketplace plan the individual chooses.
The application process involves several steps:
- Creating an Account: Individuals must first create an account on the Health Insurance Marketplace website (Healthcare.gov or a state-based Marketplace).
- Providing Information: Applicants provide information about their household size, income, and other relevant details. This includes details about their tax filing status, dependents, and any existing health insurance coverage.
- Estimating Income: Applicants must estimate their expected household income for the year. This is crucial as the subsidy amount is directly tied to income.
- Comparing Plans: Based on the provided information, the Marketplace determines the subsidy amount and displays available plans, along with their monthly premiums after the subsidy is applied.
- Enrolling in a Plan: Applicants choose a plan and enroll. The subsidy is then applied directly to their monthly premium payments, reducing the amount they pay out-of-pocket.
Cost-sharing reductions, another form of ACA assistance, further lower out-of-pocket costs for those with incomes below 250% of the FPL. These reductions can lower deductibles, copayments, and coinsurance amounts.
The amount of subsidy received varies significantly based on income.
| Income Level (as % of FPL) | Approximate Subsidy Amount (Based on a hypothetical Silver Plan premium of $500/month) |
|---|---|
| 100-150% | Premium may be close to $0/month. Cost-sharing reductions also available. |
| 151-200% | Individual pays approximately 0-2% of income for the Silver plan. |
| 201-250% | Individual pays approximately 2-6% of income for the Silver plan. Cost-sharing reductions also available. |
| 251-300% | Individual pays approximately 6-8.5% of income for the Silver plan. |
| 301-400% | Individual pays approximately 8.5% of income for the Silver plan. |
For example, a single individual with an income at 125% of the FPL might have their monthly premium substantially reduced, potentially paying close to nothing. Conversely, an individual at 350% of the FPL might still receive a subsidy, but it would be less significant, resulting in a higher monthly premium.
State-Based Programs and Other Forms of Financial Assistance
Beyond the ACA, various state-based programs and other forms of financial assistance further lower health insurance costs for specific populations or in certain circumstances. These programs often target individuals and families with unique needs or those facing specific challenges.
Many states offer Medicaid, a joint federal-state program that provides health coverage to low-income individuals, families, children, pregnant women, the elderly, and people with disabilities. Medicaid eligibility criteria and benefits vary by state, but the program typically covers a comprehensive range of healthcare services. For example, in California, Medi-Cal provides comprehensive healthcare services with minimal or no cost-sharing for eligible individuals.
Some states have also established programs to assist individuals with high medical expenses or chronic conditions. These programs might offer premium assistance, help with cost-sharing, or provide access to specialized care. For example, some states have programs to help individuals with HIV/AIDS afford their medications and healthcare.
In addition to state-specific initiatives, other forms of financial assistance may be available. Some employers offer health insurance benefits, including subsidies for their employees’ premiums. Furthermore, certain non-profit organizations and charitable groups may provide financial assistance to individuals who need help paying for healthcare.
For instance, the Health Resources and Services Administration (HRSA) provides funding for community health centers that offer affordable healthcare services, including primary care, dental care, and mental health services, to underserved populations, regardless of their ability to pay. These centers often offer a sliding fee scale based on income, making healthcare accessible to low-income individuals and families.
Analyzing the Cost Variations of Health Insurance Across Different States and Regions

Regional disparities in health insurance costs are significant, reflecting a complex interplay of local market dynamics, healthcare utilization patterns, and regulatory environments. Understanding these variations is crucial for consumers navigating the healthcare landscape and policymakers striving to improve access to affordable coverage. The cost of health insurance is not uniform across the United States.
Factors Contributing to Regional Disparities
Several factors contribute to the variations in health insurance costs across different states and regions. The local healthcare market, including the number of insurers competing for business, significantly influences premium prices. Regions with more insurance providers often experience greater competition, potentially leading to lower premiums. Conversely, areas with limited insurer choices may face higher costs. The cost of medical services, including hospital stays, physician visits, and prescription drugs, also plays a crucial role. States with higher healthcare costs tend to have higher health insurance premiums. Furthermore, the demographics of a region, such as the age and health status of the population, affect insurance costs. Older populations and those with pre-existing conditions may drive up healthcare utilization and, consequently, insurance premiums. State regulations, including mandates for specific benefits and rules regarding insurance company practices, can also impact costs. Finally, the overall economic health of a region, including factors like income levels and employment rates, indirectly affects the affordability of health insurance.
States with Highest and Lowest Average Health Insurance Premiums
Health insurance premiums vary significantly across the United States. States with higher premiums often face challenges related to healthcare costs, market competition, and population health. Conversely, states with lower premiums may benefit from factors like robust competition among insurers and lower healthcare costs.
The states with the highest average health insurance premiums often grapple with a combination of high healthcare costs, limited insurer competition, and an older or sicker population.
- Alaska: Alaska consistently has some of the highest health insurance premiums due to its geographically dispersed population, high healthcare costs, and limited competition among insurers.
- Wyoming: Wyoming faces high healthcare costs, a small and geographically spread population, and a limited number of insurance providers, leading to elevated premiums.
- Arizona: Arizona has experienced increasing healthcare costs, including hospital and prescription costs, and may face a more complex market, contributing to high insurance premiums.
The states with the lowest average health insurance premiums often benefit from robust competition among insurers, lower healthcare costs, and a younger, healthier population.
- Minnesota: Minnesota benefits from a relatively competitive insurance market, strong consumer protections, and a commitment to healthcare access, contributing to more affordable premiums.
- Rhode Island: Rhode Island has a competitive insurance market and a well-managed healthcare system, contributing to lower premiums.
- Maine: Maine benefits from a mix of factors including relatively lower healthcare costs and robust competition.
Illustration of Health Insurance Cost Variations Across the United States
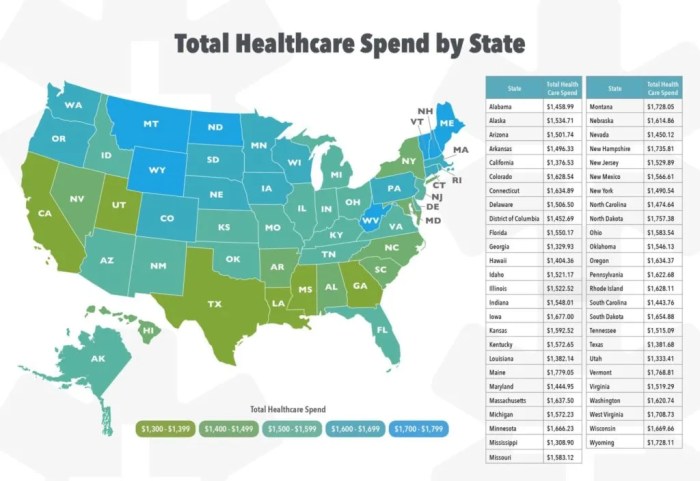
A map of the United States visually represents the variations in health insurance costs across different states. The map uses a color-coded system to indicate the average annual premium for a benchmark health insurance plan in each state. States with the highest premiums are shaded in dark red, representing the highest cost bracket. States with moderate premiums are represented by shades of orange and yellow, reflecting a gradual decrease in cost. States with the lowest premiums are colored in green, indicating the most affordable coverage. This map visually highlights the geographic disparities in health insurance costs, showing a clear pattern of higher premiums in certain regions and lower premiums in others. The legend provides a key to interpret the color-coding, indicating the range of average premiums associated with each color. This visualization helps consumers and policymakers understand the regional differences in healthcare costs and the factors influencing them. The map also helps in identifying areas where healthcare costs are particularly high or low, allowing for targeted interventions to address affordability and access issues.
Uncovering the Methods for Reducing Health Insurance Expenses
Navigating the complexities of health insurance costs can feel daunting, but several strategies can significantly reduce your financial burden. Understanding these methods empowers individuals to make informed decisions and secure more affordable coverage without sacrificing essential healthcare access. From proactive comparison shopping to leveraging wellness programs, a multi-faceted approach is key to optimizing your health insurance expenses.
Strategies for Lowering Health Insurance Costs
Several practical steps can be taken to lower health insurance costs. Careful planning and proactive engagement are crucial for achieving meaningful savings.
* Compare Plans Annually: Health insurance plans and premiums change yearly. Regularly reviewing and comparing plans on healthcare.gov or through private brokers ensures you’re getting the best value. Consider factors like monthly premiums, deductibles, co-pays, and the network of providers.
* Adjust Your Deductible: A higher deductible typically means lower monthly premiums, and vice versa. Evaluate your healthcare needs and risk tolerance. If you rarely use healthcare services, a higher deductible might be a cost-effective option. However, be prepared to pay more out-of-pocket if you need significant medical care.
* Utilize Preventive Care Services: Most health insurance plans cover preventive services like annual check-ups, vaccinations, and screenings at no cost. Taking advantage of these services can help detect potential health issues early, preventing costly treatments down the line.
* Consider a Health Savings Account (HSA): If you have a high-deductible health plan (HDHP), consider opening an HSA. Contributions to an HSA are tax-deductible, and the funds can be used tax-free for qualified medical expenses. This combination of tax benefits and cost savings can be a powerful tool for managing healthcare costs.
* Explore Cost-Saving Options: Investigate options like generic medications, negotiating with healthcare providers, and utilizing urgent care centers instead of emergency rooms for non-life-threatening conditions. These small choices can add up to significant savings over time.
Shopping for Health Insurance on Healthcare.gov
The Healthcare.gov marketplace offers a streamlined process for individuals to shop for and enroll in health insurance plans. Understanding the steps involved ensures a smooth and informed enrollment experience.
* Create an Account or Log In: Begin by creating an account on Healthcare.gov or logging into your existing account. This will allow you to access your personal information and the plan comparison tools.
* Provide Household Information: Enter details about your household, including income, family size, and any special circumstances that may affect your eligibility for financial assistance.
* Compare Plans: Use the plan comparison tool to review available plans in your area. Consider the metal tiers (Bronze, Silver, Gold, Platinum) and the associated premiums, deductibles, and cost-sharing amounts.
* Review Plan Details: Carefully examine the details of each plan, including the provider network, covered benefits, and any limitations. Ensure the plan meets your specific healthcare needs.
* Enroll in a Plan: Once you’ve selected a plan, follow the instructions to enroll. You’ll need to provide payment information and confirm your enrollment.
* Confirm Your Enrollment: After enrolling, review your confirmation materials to ensure all information is accurate. Keep a copy of your policy and know how to access your plan’s resources.
Incentivizing Healthy Behaviors Through Health Insurance
Health insurance companies often incentivize healthy behaviors to reduce healthcare costs and improve overall health outcomes. These programs can provide financial rewards and other benefits for participating individuals.
* Wellness Programs: Many insurers offer wellness programs that include health assessments, coaching, and educational resources. Participating in these programs can often lead to reduced premiums or other rewards, such as gift cards or discounts on health-related products.
* Preventive Care Incentives: Some plans offer incentives for completing preventive care services, such as annual check-ups and screenings. These incentives might include lower co-pays or premium discounts.
* Chronic Disease Management Programs: Individuals with chronic conditions like diabetes or heart disease may be eligible for disease management programs. These programs provide support and resources to help manage the condition, which can lead to better health outcomes and potentially lower healthcare costs in the long run.
* Examples of Incentives: Real-world examples include Humana’s Go365 program, which rewards members for healthy activities with points that can be redeemed for various items and services. UnitedHealthcare’s Motion program uses wearable devices to track activity and provides financial incentives for meeting certain fitness goals. These are examples that demonstrate how participation in such programs can lead to significant cost savings and improve overall health.
Closing Notes
In conclusion, the cost of health insurance is a multifaceted issue influenced by a variety of interconnected factors. From understanding the core elements of premiums to navigating the different plan types and available financial assistance, individuals can take proactive steps to control their healthcare expenses. By comparing plans, leveraging preventive care, and exploring government subsidies, consumers can make informed decisions that align with their needs and budget. Armed with this knowledge, individuals can confidently navigate the healthcare landscape and secure the coverage they need without breaking the bank.
